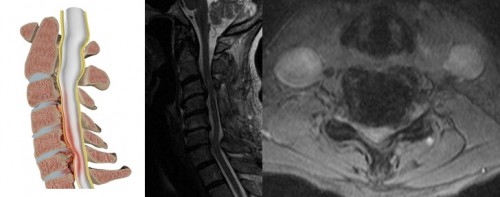
Anatomy
The lamina is the back (or posterior) part of the spinal canal. The spinal cord ends at just below the junction of the thoracic and lumbar vertebral level. Between each pair of laminae is a flat ligament called the ligamentum flavum. Therefore, the spinal canal contains the spinal cord in the cervical and thoracic spine, and nerve roots in the lumbar and sacral spine.
Why?
In the cervical spine, the most common reason to perform a laminectomy (removal of the lamina) is when the spinal cord is being compressed by bony narrowing and/or thickening of the spinal canal ligaments and/or bulging of the intervertebral discs. This condition is called cervical spondylotic myelopathy. See Myelopathy. Laminectomy is also performed to gain access to the spinal canal when a tumour needs to be removed.
When?
Patients with myelopathy may experience numbness within the tips of fingers and the hands, which may feel as though they are wearing gloves. Intricate tasks, such as writing or doing up buttons may become progressively difficult. Walking may also be affected with lower limb weakness and feeling unsteady.
The degree of the symptoms and the progression of symptoms is very variable, with some patients experiencing rapid progression and some showing no detectable deterioration.
What treatment options are there?
If your symptoms are not progressive, a wait and see approach can be adopted with regular review in the outpatients to determine the pattern of progression. If there is deterioration in the symptoms then surgery to take the pressure of the spinal cord needs to be considered. This surgery aims to prevent further progression of the symptoms, rather than cure the existing problem, although some patients do experience a degree of improvement.
The spinal cord can also be decompressed in other ways. The lamina can be opened as a trap door from the back (see Laminoplasty) or decompressed from the front, either by removing the vertebral body, (see Cervical Vertebrectomy), or by removing the discs from the front (anterior cervical discectomy and fusion).
The indications for the different types of surgery are complex and the relative benefits will need to be discussed on an individual basis.
Prior to surgery
Prior to surgery you will be explained the natural history of the condition (what is likely to happen without treatment). The surgical procedure will be explained including the postoperative care and potential complications (see Complications), prior to you consenting to undergo the operation.
Surgery
A general anaesthetic is required and once this is administered a special head clamp is applied to the skull, using three small pins, to maintain the neck in the correct position throughout the operation. The patient is positioned on their front on a special mattress to allow the surgery to be performed through the back of the neck. A surgical incision is made along the back of the neck from the base of the skull to the bottom of the neck.
Once the muscles are reflected out the way the lamina is exposed and can than be removed to relieve the pressure on the spinal cord and the nerve roots.
If the spine is unstable, (moves more than would be expected), then a fusion may need to be performed using rods, screws and bone graft.
Post operative care
There will be a drain (small tube), within the neck, which will remain there until the following morning. Patients may require a neck collar following surgery.
The following day you will be reviewed by your operating surgeon and the surgical drain will be removed. Following this you will be allowed to mobilise with the help of the physiotherapists.
The stay in hospital is very variable depending upon your general health and the degree of damage to the nerves that existed prior to surgery. Patients should expect some pain within the surgical site and it is not unusual to have aches and pains around the shoulders. You will be encouraged to mobilize as much as possible.
The skin clips should be removed at 12 to 14 days following surgery.
How long until I am better?
It will take between 6 weeks to 3 months to recover fully from the surgery, again depending on the severity of your condition. If a collar is needed it is usually worn for the first 6 weeks.